Revision Rhinoplasty and Nose Job Repair by Dr. Jose Barrera IN SAN ANTONIO, TX
When rhinoplasty doesn’t work out as expected, men and women from across the state turn to the Texas Center for Facial Plastic and Laser Surgery. Our Stanford Fellowship Trained and board-certified facial plastic surgeon Dr. Jose Barrera is one of the area’s top rhinoplasty experts. Using the latest techniques in nasal surgery, he can repair the damage to your nose and improve your rhinoplasty outcome.
Revision rhinoplasty is highly complex. Scar tissue and structural changes from previous surgeries complicate nasal surgery, already a difficult procedure. You need a surgeon with extensive rhinoplasty experience to ensure a good outcome.
Learn more about revision rhinoplasty in Texas by calling (210) 468-5426 for a consultation.
What Is Revision Rhinoplasty?
Revision rhinoplasty is a nasal surgery performed on patients that have received previous rhinoplasties. Revision surgery is considered one of the difficult types of rhinoplasty. When surgery is performed on the nose, scar tissue can develop and the underlying structure of the nose is changed. Revision rhinoplasty must repair damage and work with scarring and previously altered tissues to create a nose that is both aesthetically pleasing and structurally sound.
Revision rhinoplasty is performed for many reasons including:
- Breathing difficulties
- Rhinoplasty results that aren’t as expected
- Further refinement to the nose after nasal surgery
- Facial trauma or injury after a previous rhinoplasty
If you’ve had a previous rhinoplasty and are considering additional nasal surgery, contact our office to learn more about revision rhinoplasty in San Antonio.
What Happens During Revision Rhinoplasty in San Antonio?
From breathing problems to aesthetic changes, revision rhinoplasty is performed for many reasons. As such, the procedure varies considerably. Dr. Barrera will create a customized plan for your surgery, designed to address your specific concerns. For detailed information about what to expect, talk with Dr. Barrera.
Revision rhinoplasty is often performed using an open technique. Open rhinoplasty provides better visualization and access to your nose. An incision will be created along the columella, the tissue that divides the nostrils, and the skin is lifted. Dr. Barrera will shape and refine the nose. Cartilage grafting is often needed in revision rhinoplasty.

Patients undergoing revision rhinoplasty may have dorsal irregularities which correspond to nasal bone asymmetry and residual boney humps, inverted V deformity from loss of support to the upper lateral cartilages, or pollybeak deformity from excessive scar tissue in the lower portion of the nose. Reconstruction using septal cartilage, ear grafts, and costal cartilage or rib grafts may be necessary. After surgery, the nose is placed in a protective splint to hold refinements in position until they have healed. Patients spend a few hours in recovery with careful monitoring by our skilled nursing team before heading home.
What Can You Expect During Revision Rhinoplasty Recovery?
After rhinoplasty, your nose may feel bruised, swollen, and tender. Swelling is very common after revision surgery and tends to be more pronounced than after a first-time rhinoplasty. Plan on taking about a week off from work.
Our patients recover quickly. After the first day, many can resume basic daily activities. Take it slowly and reintroduce activity as you’re comfortable and able.
To ensure comfort, we’ll provide prescriptions for analgesic pain medications and antibiotics. We ask patients to irrigate the nose with saline during recovery.
Dr. Barrera will provide detailed recovery instructions and is available if you have questions or concerns. We’ll schedule several follow-up visits. These visits allow us to assess your healing. They are an essential part of the recovery process. Make every effort to attend your follow-up visits.
- Sutures and splints are typically removed five to eight days after surgery.
- Avoid strenuous exercise, heavy lifting, and blowing your nose until you’re cleared by Dr. Barrera.
- The nose is highly sensitive to the sun after rhinoplasty. Avoid sun exposure.
Careful attention to our recovery instructions is essential to achieving your desired result after this procedure.
There are many common rhinoplasty concerns. These concerns may be due to over-resection of the underlying nasal cartilages or abnormal healing with scar. Other patients present with complications after their rhinoplasty surgery.
What Conditions Can Revision Rhinoplasty Treat?
Septal Perforation
Septal perforations can be caused by trauma, infection, autoimmune, inhalant drugs, malignancy or prior rhinoplasty surgery. When indicated a biopsy may be needed to evaluate the cause of the perforation. Dr. Barrera will perform a nasal endoscopy to evaluate the extent of the perforation.
Patients often present with crusting and bleeding from the nose as well obstruction and whistling noises. Surgical correction is indicated when failed medical management cannot decrease these symptoms. An interpositional graft made from ear or costal cartilage and mucosal flaps are often necessary.
Treating the Crooked Nose


Crooked noses can be caused by trauma, facial asymmetries or prior rhinoplasty. Correction of the crooked nose requires complete dissection of the nose often through an open approach. Correcting the deviated septum is the first step, followed by osteotomies and spreader grafts for the middle area of the nose. Nasal tip deviations can be addressed using caudal extension grafts and reshaping the nasal tip cartilages.
Lengthening the short nose

The shortened nose can be caused by concavity of the dorsum or overresection of a boney hump, over-rotation of the nasal tip, deep nasion, and an obtuse nasolabial angle. Treatment requires open rhinoplasty with complete release of the supporting structures, caudal extension grafts, extended spreader grafts, radix grafts, and possibly tip grafts to lengthen the nose. All of these cartilage grafts can be fashioned from septum, ear, or costal cartilage (rib) grafts.
The Tension Nose and Treating the Long Nose

Patients with an extremely long caudal septum with overprojection of the nasal tip and weak tip cartilages often have a tension nose. Patients present long noses where the nasal tip descends below the dorsum of the nose. Treatment involves reducing the dorsal septum to deproject the nose while supporting the remaining septum with spreader grafts and a caudal extension graft. The long columella can be treated with a tongue in groove technique of the columella cartilage or caudal extension graft. Alar base flairing can be treated with base reduction of the nose with a Weir or combined Sill excision.
Pollybreak Deformity treatment

Patients with a pollybeak deformity present with overprojection of the lower nasal dorsum due to loss of tip support, scar building, or inadequate cartilage reduction of the dorsum. Treatment is directed to remove excessive scar and provide lower nasal support using spreader grafts and caudal extension graft. Sometimes defatting the SMAS layer is necessary. Taping and steroid injections are often necessary.
Saddle Nose Deformity

The saddle nose deformity is caused by over-resection of the nasal dorsum with loss of the natural height of the nose from prior rhinoplasty. Other causes include autoimmune diseases like Wegeners granulomatosis, relapsing polychondritis, or cocaine abuse. Overuse of topical nasal decongestants can also cause saddle nose deformity. Treatment includes spreader grafting, onlay grafts to restablish dorsal height, and nasal tip support using costal cartilage grafting.
Inverted V Deformity

The inverted V deformity is often seen in revision rhinoplasty. Patients present with collapse of the upper lateral cartilages leading to depression in the mid vault of the nose from over-resection after hump removal. Spreader grafts are often necessary. Increase risk of inverted V deformity occurs in patients with short nasal bones and long upper lateral cartilages.
Over-resection of the Lateral Crura

The lateral crura are the nasal tip cartilages that offer support to the nasal valve of the nose. Patients who receive cosmetic rhinoplasty with resultant over-resection of the lateral crura can have atypical pinched nasal tips, supraalar collapse, asymmetry, bossae formation, and alar retraction. Dr. Barrera typically preserves 7 – 8 mm of the lateral crura when performing cephalic trim in order to avoid alar retraction. In alar retraction, alar batten grafts, lateral crural strut grafts, and alar rim grafts may be using to redefine and support the nasal tip.
Bossae Deformity


In bossae deformity, knuckling of the lower lateral cartilage results in visible and palpable nasal tip asymmetry. Patients with thin skin, strong alar carilages, and tip bifidity as predisposed to bossae deformity. Treatment involves trimming the bossae, obtaining good nasal tip structure and symmetry, and onlay camouflaging using crushed cartilage techniques.
Hanging Columella

A hanging columella is due to failed correction at the time of previous rhinoplasty surgery. Patients with a hanging columella benefit from tongue in groove technique using the native septum or a septal extension graft for support. Removal of the membranous septum may also be helpful.
Open Roof Deformity and Rocker Deformity
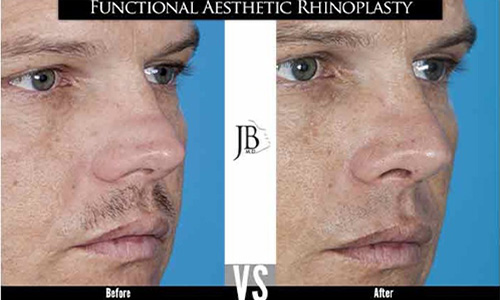
The open roof deformity is caused by inadequate lateral osteotomies or failure to perform osteotomies after dorsal hump reduction. Irregularity of the bridge of the nose and dorsum can result with indentations. Spreader grafting and osteotomies are necessary. Similarly, rocker deformity results from carrying the osteotomy too high resulting in lateral displacement of the superior fracture. A transverse percutaneous osteotomy can alleviate this problem.
Nasal Valve Obstruction
Nasal valve obstruction may be caused by previous rhinoplasty surgery or by inadequate cartilage of the external valve. Patients may also present with airflow limitations due to a narrow internal valve.
Patients often say that pulling the nasal ala with their fingers, called the Cottle maneuver, improves nasal breathing. Using cotton tip applicators, the modified cottle maneuver can help to further identify whether internal or external valve compromise exists.

Treating the External Valve and Caudal Septal Deviation
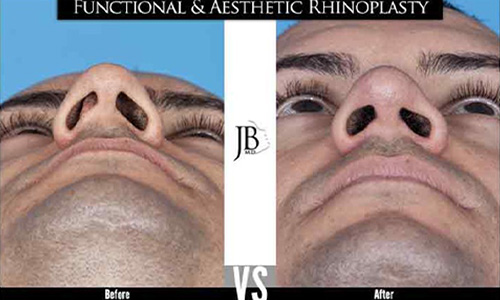
Patients with external valve collapse present with either collapse of the lower alar cartilages, narrowing of the base of the nose or nasal sill, a columella asymmetry, or a caudal deviation of the nasal septum. The caudal septal deviation is a common finding in sports injuries, trauma, and previous unsuccessful septoplasty. Dr. Barrera utilizes additional grafting in the form of septal extension grafts, alar batton grafts, and / or lateral crural strut grafts to treat the external valve.
A common presenting complaint by patients to otolaryngologists is trouble breathing through the nose. While etiologies are numerous, nasal valve stenosis is commonly implicated in these patients. Patients worry about their ability to obtain appropriate oxygen, especially during times of exertion, as well as quality of sleep. In particular, this type of nasal deformity may worsen a patient’s obstructive sleep apnea and contribute to excessive daytime sleepiness. Nasal valve incompetence is commonly a quality of life problem for patients. Surgeries have been developed to address such issues and are aimed at correcting internal and external nasal valve structure as well as creating space in the nasal passage. These techniques involve grafting cartilage from the existing nasal septum or from other parts of the body, such as rib or ear. Current literature often uses the umbrella term functional rhinoplasty to describe these operations.
Nasal Valve Obstruction and Internal valve correction


Nasal Valve obstruction is common in patients with previous rhinoplasty surgery. At the time of revision rhinoplasty, care must be taken to ensure the internal valve is improved by proper placement of spreader grafts and a thorough septoplasty to treat a high septal deviation. The middle vault must be supported to ensure that ongoing collapse does not recur.
Surgeries to correct nasal valve insufficiency that follows septoplasty with rhinoplasty using alar batton grafting or lateral crural strut grafts, and turbinate outfracture are very common. While these techniques have shown promise for patients seeking relief for nasal obstruction, they are invasive, and depending on the patient’s past surgical history, may be complicated.
An alternative approach has been introduced by Spirox with its novel nasal device, Latera. This absorbable implant serves to support the nasal cartilage in a way that does not require cartilage harvest and reshaping as does traditional methods. Spirox Latera is an innovative device that is FDA approved for support of the lateral nasal wall in patients with nasal valve incompetence. Of important note, the implant does not alter the patient’s normal nasal architecture, and thus the aesthetics of the nose may be preserved.


Patients often seek ways to improve their health in ways that least disrupts their daily lives. Latera implant may offer a solution for people seeking minimally invasive correction of nasal valve stenosis and collapse. In this study, we aim to investigate the effect of Latera implant versus traditional functional rhinoplasty on nasal airway obstruction through subjective scales and polysomnogram data. This research may be of importance to clinicians seeking to offer their patient’s the best options for treatment.
What Is Non-Surgical Revision Rhinoplasty?

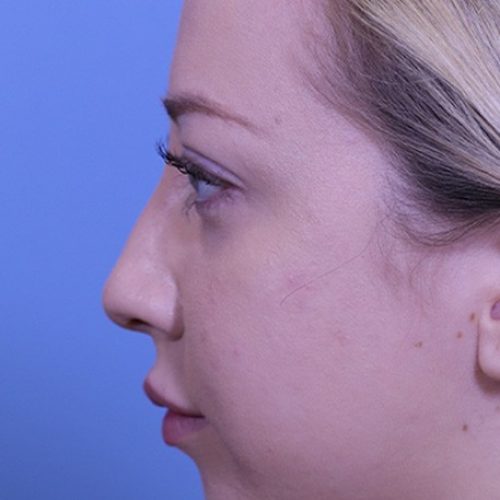
Many patients don’t want additional surgery but wish they could improve their rhinoplasty results. You may be a candidate for non-surgical correction of depressions and humps on the nasal bridge. Non-surgical correction is also used to refine the tip of the nose.
Non-surgical rhinoplasty uses dermal fillers such as Restylane to change the appearance of the nose and create a more attractive shape. Fillers aren’t permanent, but they are long-lasting. Results last from three months to two years, depending on the filler used and the area treated.
If you have breathing obstructions or structural issues with your nose, surgery is needed. Non-surgical rhinoplasty is limited in what it can achieve, but it does help many of our patients to avoid revision surgery while improving their rhinoplasty results.
Revision Rhinoplasty in Texas: Frequently Asked Questions
Few plastic surgeons in Texas have the training and experience that Dr. Barrera does, especially when it comes to nasal surgery. Dr. Barrera is board-certified in otolaryngology, a medical specialty that focuses on the ears, nose, and throat. He is also a board-certified facial plastic surgeon. He is highly experienced in nasal surgery and has performed many complicated revision procedures with excellent results.
If you’re unhappy with the results of your previous rhinoplasty, you may be a candidate for revision surgery. We recommend that patients wait at least a year before revision surgery. Ideal candidates are in good health and have realistic expectations for the procedure. To find out if you’re a candidate, contact Dr. Barrera for a consultation.
Revision rhinoplasty typically takes more time than a first-time rhinoplasty. Procedures can take four hours or more, compared with one to two hours for a first-time rhinoplasty.
Revision rhinoplasty is often performed using an open technique. A small incision is created outside of the nostrils on the columella. Most patients don’t notice the scar after healing.
Come to your consultation with a firm idea of what you hope to achieve. Be prepared to discuss with Dr. Barrera what went wrong on your previous rhinoplasty. Bring along a list of questions. We look forward to meeting with you and helping you achieve your rhinoplasty goals.
Adherence to proper rhinoplasty principles is paramount in obtaining an aesthetically pleasing and functional result. A bad nose job can be fixed by following these guidelines. Dr. Barrera specializes in rhinoplasty and revision rhinoplasty surgery to fix a bad nose job.
Success rates for revision rhinoplasty approximate 85%. The reported incidence of complication after rhinoplasty surgery is between 8-15% in the medical literature. It is the surgeon’s responsibility to have a detailed knowledge of the anatomic variants encountered in revision rhinoplasty.
You can tell if you need a revision rhinoplasty if there is a deformity which causes aesthetic deviations or nasal airway obstruction. Some of these abnormalities are secondary to healing and scarring while others are due to over-resection of the nasal cartilage and bone. These include pollybeak deformity, saddle-nose deformity, inverted V deformity, over-resection of the latera crura (nasal tip cartilages), bossae of the nasal tip, alar retraction, hanging columella, vestibular deformity, and open roof deformities. Dr. Barrera recommends a consultation with a board certified facial plastic surgeon for evaluation and a treatment plan. We recommend visiting our gallery at www.drjosebarrera.com to view our results with treating these common deformities from previous rhinoplasty surgery.
There are no age requirements to undergo a revision rhinoplasty surgery. If a deformity exists or nasal obstruction remains a concern, then the patient is a candidate. A history and physical, appropriate lab work, and possibly an EKG may be necessary.
Nose jobs fail due to unforeseen circumstances like scarring or from a lapse of structural support when performing the primary rhinoplasty. Inadequate cartilage removal at the anterior septal angle or supratip scar formation can both lead to a pollybeak deformity. Treatment is directed to the cause of the problem. Revision rhinoplasty then addresses the cartilage to support the nasal tip, middle vault, and correct nasal bony abnormalities. Sometimes a nonsurgical approach with interval steroid injections and skin taping is needed. Other patients may need another rhinoplasty surgery.
Patients may also present with autoimmune conditions such as Wegners Granulomatosis, relapsing chondritis, cocaine abuse, and chronic use of nasal decongestants which further promote a nasal deformity. Medical diagnosis and control of the condition is paramount to obtaining a successful outcome.
The risks of revision rhinoplasty include further nasal obstruction, inability to remove all the scar tissue, inability to fully support a previous loss of cartilage, persistent asymmetry, and inability to camouflage a deformity due to poor skin or very thin skin.
Plastic surgeons who regularly perform rhinoplasty surgery may also perform revision rhinoplasty surgery. However, a revision surgery is not the same as a primary rhinoplasty. The use of additional grafting material from the septum, rib, and ears and well as other harvesting materials from the scalp may be necessary to revise a nose. Dr. Barrera recommends surgeons with knowledge of common rhinoplasty complications and their etiology. Often a plastic surgeon or facial plastic surgeon with rhinoplasty practices are good resources for revision nose job care.
At Texas Center for Facial Plastic and Laser Surgery, Dr. Barrera performs all his rhinoplasty surgeries using Total intravenous anesthesia (TIVA). TIVA is a technique of general anesthesia which uses a combination of agents given exclusively by the intravenous route without the use of inhalation agents.
Revision rhinoplasty surgery may involve a septoplasty, however a septoplasty by itself will not change the aesthetic qualities of the nose. Therefore, septoplasty surgery is not considered a revision rhinoplasty.
In Texas, the average revision rhinoplasty cost is approximately $9000-15,000 including anesthesia and hospital fees. Surgery may require cartilage grafting from rib (costal cartilage), septum, or ear cartilage which extends the time, cost, and complexity of the surgery.
Revision rhinoplasty is more expensive than primary rhinoplasty due to the added complexity of the surgery, thus requiring added expertise, operating room time, anesthesia, and need for harvesting additional grafts such as septum, costal (rib) cartilage, and auricular (ear) cartilage.
A revision rhinoplasty is not usually covered by insurance since it is considered a cosmetic surgery. Patients with nasal airway obstruction from a persistent deviated septum or nasal valve collapse can be authorized by insurance for coverage to correct the site of obstruction. However, any portion of the surgery that changes the aesthetic portion of the nose is considered cosmetic in nature, therefore, not covered.
Dr. Jose Barrera, MD, PLLC, dba Texas Center for Facial Plastic and Laser Surgery, and Endormir Surgical, PLLC accept most major insurance. Financing is available through CareCredit® and Prosper Lending. To apply for financing click here and go to the “Apply Now” button. For CareCredit®, additional information may be found below.
CARECREDIT®
CareCredit® offers a line of credit that may be applied to copays, deductibles, as well as other costs not covered by your insurance.
Designed specifically for the payment of healthcare services, CareCredit® functions like a credit card, offering the flexibility and convenience of making payments over time.
Visit CareCredit® to apply and schedule your consultation today!
A broken nose after a primary rhinoplasty doesn’t always mean you need a revision rhinoplasty. A closed nasal reduction can be performed to reduce the nasal fracture if done in the first 10 days after injury. After 3 weeks, the bones begin to heal in the fractured position and a revision rhinoplasty may be necessary.
There are signs of a bad nose job. The crooked nose may show minor or major asymmetry. Careful facial analysis will reveal these persistent abnormalities. Sometimes a crooked nose may be due to trauma. While obtaining a completely straight nose may be impossible, camouflaging and deconstruction and reconstruction surgery may be necessary.
Other signs include a tension nose where the nasal tip overprojects due to an overdeveloped and long caudal septum. The septum may not be addressed in the primary rhinoplasty leading to this problem. Treatment includes dorsal septal reduction, spreader grafts, and tongue in groove maneuvers.
Grafts may become visible in patients with thin skin and may have to be removed. Other patients have alloplastic implants made from silicone, gortex, or medpor. The ideal synthetic implant should be noninflammatory, noncarcinogenic, nonallergic and adapt to shape and integrate with the nose. No alloplastic implant has been developed that abides by all these properties. Dr. Barrera has replaced several silicone nasal implants with a diced cartilage glue graft made from costal cartilage. See our results in the gallery.
After a rhinoplasty, it is recommended to wait one year before getting a revision rhinoplasty. Treatments such as steroid injections, taping, massage, and 5-fluorouracil may be used in the interim to reduce swelling. Some patients have very thick skin which blunt nasal tip definition. The use of isotretinoin has been deemed as an appropriate treatment for patients with thick skin after 6 months from their rhinoplasty. Patients with small dorsal irregularities can have a revision hump take-down after 6 months in select cases.
Revision rhinoplasty surgery is performed through an open approach. A transcolumellar incision is made and combined with marginal incisions. Direct exposure and inspection of the nose can be performed. Precise modification and stabilization of the nasal tip and dorsum can be achieved through an open approach.
A revision rhinoplasty usually takes between 3-6 hours to perform. Cartilage grafts are harvested during this period and tip and dorsum modifications with graft placement and osteotomies are performed.
The revision rhinoplasty recovery is similar to a primary nose recovery. Dr. Barrera advises patients that it will take one year for 90% of the swelling to diminish. Favourable results are often seen at 1 month postoperative, but the final result may be achieved after 3 years.
Speeding up recovery after rhinoplasty surgery is similar to other surgeries. Proper nutrition, hydration, wound care, and sleep are all necessary for good healing. Avoiding exercise and lifting over 10 lbs for one month is recommended. Proper skin care and UVA / UVB physical defense sun block is a must.
Visible scars are minimized in revision rhinoplasty. A transcolumellar incision is made and sometimes a small incision is made for a transverse osteotomy to reduce overly wide nasal bones. However, skin thickness is a limiting factor to refinement after rhinoplasty. Thick skin is inelastic and requires special attention in the postoperative period including proper skin care, UV avoidance, and possibly measures to reduce the sebaceous quality of the nose. Thin skin can reveal small imperfections in the postoperative contour of the nose. Scarring beneath the skin can also blunt the postoperative result. Dr. Barrera examines his patients in regular intervals to evaluate the quality of the skin and its healing.
Revision rhinoplasty is seldom painful. Dr. Barrera has completed a clinical trial evaluating the use of non-narcotic medications for postoperative pain management in rhinoplasty patients. Dr. Barrera prefers not to use opioid medications after revision rhinoplasty.
Revision rhinoplasty is considered a major operation. Even though patients often feel well enough to drive home, Dr. Barrera recommends a driver and an attendant during the first night after surgery.
Stitches are removed after one week after revision rhinoplasty surgery. Good skincare is warranted after suture removal.
Although good results are expected, there is no guarantee or warranty expressed or implied, on the results that may be obtained. Patients seeking revision rhinoplasty surgery may be disappointed with the results of tip rhinoplasty surgery. This would include risks such as asymmetry, loss of function, structural malposition, unacceptable visible or tactile deformities, asymmetric nostrils, unsatisfactory surgical scar location, poor healing, wound disruption, and loss of sensation. It may be necessary to perform additional surgery to attempt to improve your results.
Revision rhinoplasty surgery is considered successful when aesthetic deformities are improved and nasal breathing is restored. It is important that all patients seeking to undergo elective surgery have realistic expectations that focus on improvement rather than perfection. Complications or less than satisfactory results are sometimes unavoidable, may require additional surgery and often are stressful. Please openly discuss with your surgeon, prior to surgery, any history that you may have of significant emotional depression or mental health disorders. Although many individuals may benefit psychologically from the results of elective surgery, effects on mental health cannot be accurately predicted.
Patients who experience complications after revision rhinoplasty surgery should seek the opinion of their surgeon. Follow all physician instructions carefully; this is essential for the success of your outcome. It is important that the surgical incisions are not subjected to excessive force, swelling, abrasion, or motion during the time of healing. Personal and vocational activity needs to be restricted. Protective dressings and splints should not be removed unless instructed by your plastic surgeon. Successful postoperative function depends on both surgery and subsequent care. Physical activity that increases your pulse or heart rate may cause bruising, swelling, fluid accumulation and the need for return to surgery. It is wise to refrain from intimate physical activities after surgery until your physician states it is safe. It is important that you participate in follow-up care, return for aftercare, and promote your recovery after surgery.
Do you need revision rhinoplasty in San Antonio, TX? Dr. Jose Barrera is one of the area’s top surgeons for this procedure. Contact our office to learn more or schedule a consultation.

















